Troubling Vital Signs for Bright Health
On paper, Bright Health Group was an investor’s dream.
Led by experienced health insurance execs, the company promised a new approach. From early on, Bright touted a “narrow network” philosophy that worked closely with a small group of providers. The company’s target market wasn’t large employers or institutions; instead, it looked to sell individual health plans through the Affordable Care Act (ACA) exchanges, as well as Medicare Advantage plans for older Americans. Bright leaders heralded a new technology platform that would make the claims process easier for providers and patients alike.
At its peak, Bright was valued at $11.2 billion, cementing its status as Minnesota’s first “unicorn” startup—a company valued at over $1 billion. It earned praise and recognition from startup boosters and investors, and even counted high-profile figures like Andy Slavitt, who ran Medicare and Medicaid in the Obama administration, on its board of directors.
In a 2021 prospectus ahead of its eye-popping $924 million initial public offering that year, Bright noted that the company was serving more than 623,000 consumers across 14 states.
“We believe the U.S. health care system is broken,” Bright officials wrote. “Since its inception, Bright Health has proven, expanded, and enhanced our aligned enablement model.”
The company in that document bears little resemblance to the one that exists today. As of the start of 2023, Bright has completely pulled out of the insurance business in all but one state. It’s exited the market for ACA plans and is instead focused exclusively on Medicare Advantage in California, alongside limited primary care offerings. It faces delisting on the New York Stock Exchange, and it still hasn’t turned a profit. Meanwhile, the status of Bright’s much-promised technology platform remains unclear, and its clunky claims processing system has aroused the ire of regulators.
Business students are likely to study Bright Health’s rise and fall for years to come. In the interim, many are wondering exactly where and how things went wrong. Ari Gottlieb, principal with Chicago-based health care consulting firm A2 Strategy Group, offers a succinct response: “I think the one-word answer that I would give would be ‘Hubris.’ ”
Indeed, in the end, the company was brought down not by Wall Street or the pandemic, but by a deeply flawed operational model, difficulties marketing a new insurance product, and leaders’ growth-at-all-costs mentality, according to interviews with health insurance experts and company insiders. Bright attracted and subsequently burned through a large sum of capital, along with many smart people with good intentions, while causing headaches for customers.
In some ways, going public simply laid bare Bright’s serious operational deficiencies. According to former employees and industry experts, Bright lacked the infrastructure to handle the most basic elements of health insurance, such as claims processing. The company also lacked name recognition in the markets where it opened.
That all meant consequences for both Bright and its customers. This past April, Colorado regulators slapped Bright with a $1 million fine, in part for failing to pay claims in a timely manner. At the time, the Colorado Division of Insurance said it had received more than 100 complaints about Bright that “indicated systemic operational problems.”
Notably, Colorado was the first state where Bright sold insurance. The company began selling health plans there in 2017, two years after its founding.
As of early January, Bright is a shell of its former self. Today, the company’s only remaining insurance offering is Medicare Advantage in California. Medicare Advantage is essentially government-backed health insurance facilitated by an outside company, and is considered a lucrative business.
 Repackaging the HMO model
Repackaging the HMO model
Bright’s narrow network strategy wasn’t necessarily a novel idea; health maintenance organizations have long operated under a similar premise. Where Bright looked to differentiate itself was in technology. The company long billed itself as a “technology-enabled, value-driven health care company.”
In a 2018 article, co-founder Bob Sheehy told TCB that “the long-term issues that we have in health care are basically caused by the status quo.”
Yet it’s still not clear whether the company’s platform was ever fully developed. Multiple former employees told us the technology that underpins Bright is more hype than code.
Through a spokesperson, Bright declined to answer specific questions relating to its technology. In its prospectus, company officials described two main technologies: Consumer 360, a platform to aggregate clinical and administrative data, and the Bright Health Intelligent Operating System, an “end-to-end intelligent technology platform [composed] of consumer, care delivery, and administrative solutions.”
Read more from this issue

Auspicious starts
A trio of Minnesota founders with impressive credentials launched Bright Health in 2015. Sheehy, who served as CEO for a time and remains chairman, was CEO of UnitedHealthcare until 2007. Kyle Rolfing had launched two other health-related startups, while Dr. Tom Valvidia brought a physician’s vantage point.
Together, the three men seemed to have all the knowledge needed to build a new model. Bessemer Ventures, an early investor that still holds a significant number of shares, had only positive things to say at the start.
“The investment thesis here is simple—huge market, great team, and a strong initial health plan product with many expansion opportunities,” Bessemer wrote in a 2016 memo. “Bright Health is playing in one of the biggest markets within health care (and probably within venture) and is also led by an A+ CEO (Bob Sheehy) that we think is one of the better people out there to start a new health plan. Bob has operated more health plans than anyone else in the country.”
In 2017, Bright began selling its first insurance products, in Colorado. Over the next few years, the company expanded rapidly as it pulled in hundreds of millions of dollars from investors. Bright expanded to Alabama and Arizona in 2018, then came Tennessee, Ohio, and New York in 2019. Curiously, the company never sold insurance in Minnesota, the state it’s headquartered in.
Bright’s biggest expansion came in 2020, when it began selling insurance in seven new states. It dipped its toe into California—and Medicare Advantage—through its acquisition of Brand New Day, a provider of Medicare Advantage plans in the state. “This transaction gives Bright Health Plan a strong presence in California with an established and philosophically aligned partner,” said Bright’s current CEO G. Mike Mikan, who was president and vice chair at the time.
As the company continued to expand, investor dollars flowed in. At the end of 2019, Bright pulled in a $635 million Series D raise. In September 2020, the company landed another $500 million, bringing its total raised to more than $1.5 billion.
Yet despite the promises Bright made to investors and patients, the company’s foray into other states might have happened too quickly for its own good. The health insurance business varies widely from state to state; each has its own rules and regulations, as well as unique population needs. In Minnesota, for instance, until 2017 HMOs had to be nonprofits.
“It is safe to say that when you’re trying to break out and establish a market presence and gain market share in 15 or 20 different states at a time, you have to work very carefully with state regulators,” says Allan Baumgarten, a Minnesota-based independent health analyst. “Maybe it’s possible to say they bit off more than they could chew, that they maybe should have taken a more measured approach.”
But Bright’s leadership seemed hell-bent on raising the company’s valuation ahead of an eventual IPO, whatever the cost. “The first big mistake was this hyper-growth focus,” says Gottlieb. “In preparation for an IPO, they started aggressively expanding to more and more markets.”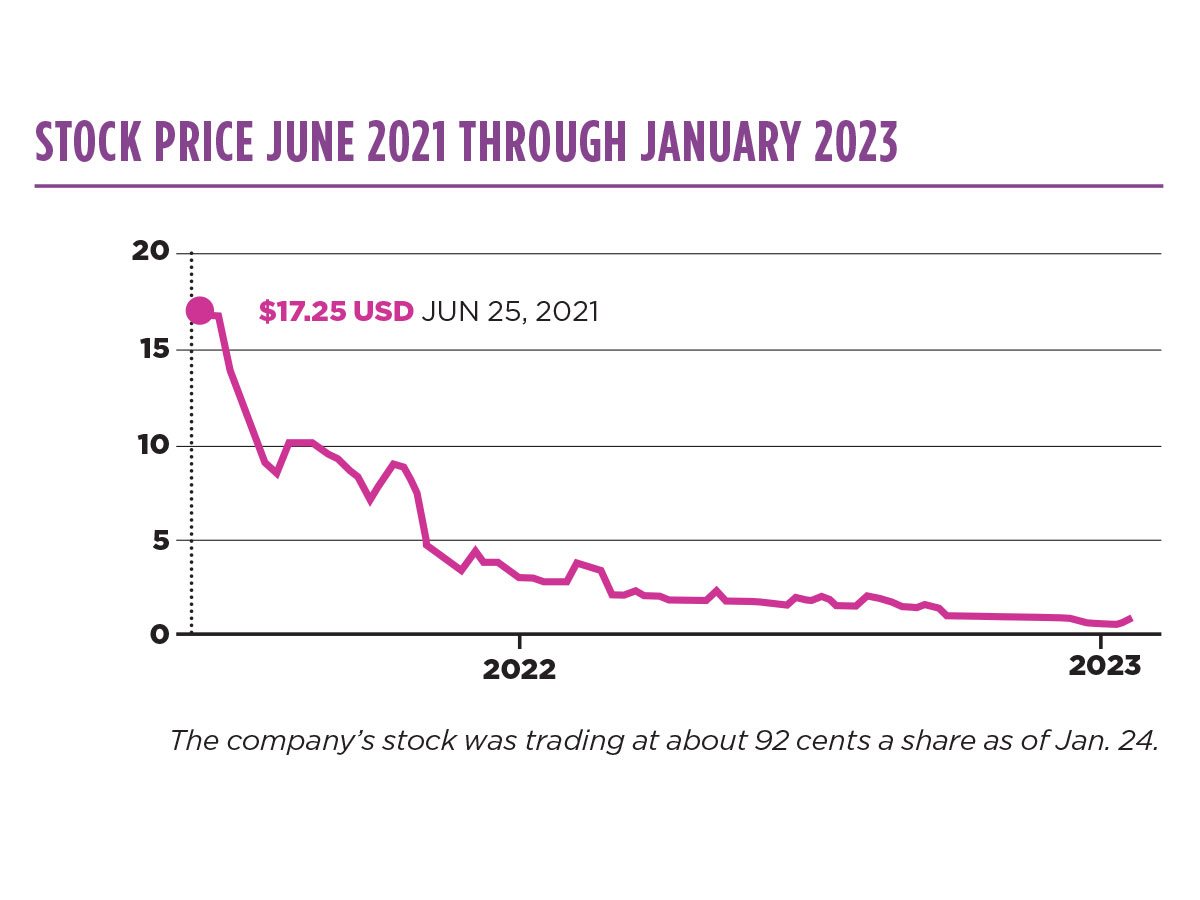
Growth at all costs
On June 24, 2021, Bright execs were all smiles as CEO Mikan rang the closing bell at the New York Stock Exchange. There was a lot to smile about at the time. The company had just completed its IPO, adding nearly $1 billion to its coffers. At $924 million, Bright’s was the largest IPO in Minnesota history.
The company priced shares at $18, though traders ended up buying around $17.25 a share. The value of Bright’s stock has plummeted since then. As of Jan. 24, it was trading at 92 cents a share.
A month earlier, Bright was warned it could be delisted from the NYSE for failing to meet the minimum price of $1 a share for 30 consecutive days. Bright officials signaled their intent to “cure the deficiency” and avoid delisting, yet the stock price remains below $1 at press time. (The warning came after Bright laid off 99 employees.)
Bright’s fumbles have given investors pause. In a Nov. 8 note, J.P. Morgan analysts said Bright “needs to string together several quarters of consistent performance in order to restore investor confidence.”
“Persistent execution hiccups since going public give us concern about the sustainability of the business,” they added. “We think other companies in our coverage offer exposure to Medicare Advantage and/or primary care with a more balanced risk/reward.”
 Trouble finding traction
Trouble finding traction
To be sure, building a new health plan from scratch is not easy. Consider the fates of fellow health insurance upstarts Oscar Health and Clover Health. Both began trading publicly in 2021, the same year as Bright, and both have seen their stock tank.
Generally speaking, it’s tough to compete with established brands in the space, such as UnitedHealth Group, Blue Cross Blue Shield, Humana, and others. They’re the entities with the capital and scale to grow.
Traditional insurers also have the means to build the type of system that Bright had been looking to create. “The only players that really have a bead on doing the type of comprehensive care management that Bright promised are the ones that, for better or worse, have been entrenched forever—the old-school HMOs,” says Stephen Parente, professor of finance at the University of Minnesota Carlson School of Management. “They have what Bright was [angling for]: complete control over provider community.”
Bright’s leaders have long said their aim was to create deep partnerships with health care providers in the communities they entered, but as a newcomer, it was hard to gain any real traction. “As a new brand name, it takes a while to build up recognition,” says Baumgarten.
Breaking into the Medicare Advantage market also had its challenges; though it may have appeared lucrative at the outset, with big names like AARP and UnitedHealth Group already dominating the space, it’s been a tough market to break into.“When you’re trying to disrupt something and the market is still functioning halfway decently,” Parente says, “it’s challenging.”
Plus, consumers generally don’t have a high opinion of health insurance companies. They’re generally seen as third-party entities that consumers only think about when they’re absolutely needed.
“Patients generally don’t have trust in insurance companies,” Parente adds. “They do have trust in their providers, but they just want a third party that’s going to help them pay for things they can’t pay out of cash.”
“Maybe it’s possible to say they bit off more than they could chew, that they maybe should have taken a more measured approach.”
—Allan Baumgarten, a Minnesota-based independent health analyst
A troubled culture
The image that Bright portrayed to investors was a stark contrast to the company’s internal culture. Former employees describe a difficult and at times hostile workplace; none would speak on the record for fear of retaliation. Some cited shouting matches in the C-suite. One former worker said the company was “a cultural cesspool,” another said there were instances of misogyny. Several said there was no room for questioning, either.
Through a spokesperson, Bright declined comment.
Startup culture is, of course, rife with stories of volatile workplaces. Often, a positive culture is sacrificed in the name of growth. San Francisco-based ride-hailing app Uber, for instance, was the subject of a yearslong investigation by the Equal Employment Opportunity Commission for widespread claims of sexual harassment among corporate staff. In 2019, Uber agreed to a $4.4 million settlement for employees who experienced sexual harassment at the company.
What’s next?
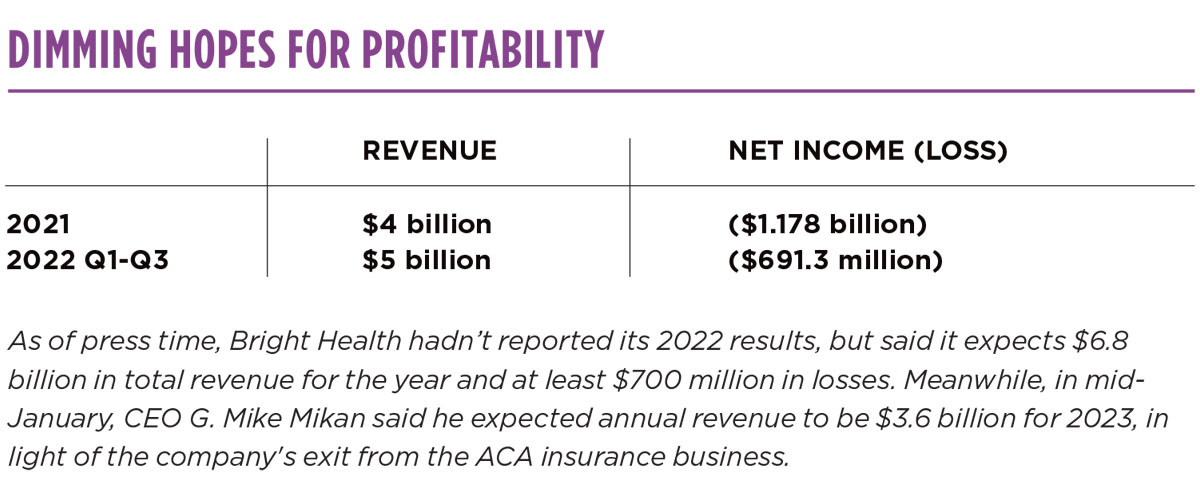
Bright’s leaders remain sanguine about the company’s long-term prospects. In early January, when the stock was trading at 80 cents, Bright said it expected revenue between $3.4 billion and $3.6 billion in 2023. Though the company hadn’t reported its 2022 year-end results as of press time, Bright said it expected $6.8 billion in revenue, with a loss of up to $700 million.
Through a spokesman, Bright said it plans to “focus on maximizing the efficiency and effectiveness of the fully aligned care model” in the new year.
“Through its scaled, value-driven care model, Bright looks forward to serving the health needs of the aging and underserved populations, delivering improved outcomes and lower costs for consumers and its partners,” the spokesman said in an email.
Speaking at the 41st J.P. Morgan Healthcare conference on Jan. 11, Mikan said he’s “never been more excited” about the company’s future. With a “sharpened focus,” Bright is set to achieve profitability in 2023. “The business we’re presenting today,” he told attendees, “takes the best of Bright Health and removes the volatility of the ACA insurance business, doubling down on the segments of the business where we can create the most value.”
Whether Bright’s new orientation will lead to profitability and growth is up for debate. In the meantime, there are a few off-ramps left for Bright. Acquisition by another company is one.
Bright exists today with a trail of spurned executives and disappointed patients in its wake, and its future remains unclear. “They’ve salvaged what they can,” Gottlieb says. “Bright’s legacy will more than likely be one of spectacular implosion and failure, than of success.”









