Getting Your Order Right Could Be a Matter of Life or Death
When I get a hankering for fast food, I usually go to Burger King. It’s not so much because I like Burger King (though I do prefer it to McDonald’s or Wendy’s for a burger). I go there because they always get my order right.
I could have any combination of three kids, a spouse and a dog in the car, all yammering or barking in my ear about what they want. Yet no matter how particular they are with their menu choices, the right food in the right quantity is always in the bags. And I appreciate it. Those of you who are parents know the grief that comes with a cheese Whopper with everything that was supposed to be plain.
I don’t have the same level of confidence in my local pharmacy. Although I use it to fill my prescriptions, I think the fact that the pharmacists and technicians there have never screwed up my order is more a matter of luck than skill. When you can ring up an antibiotic and a frozen pizza at the same register, it makes me a little suspect.
A number of recent reports and research articles suggest that medication errors—whether at the pharmacy, physician’s office or hospital—are more common than most of us believe. For employers who offer prescription drug benefits to their workers, the situation should be of concern. In the best-case scenario, you’re paying for the wrong order. In the worst-case scenario, you’re paying to recruit a replacement for an employee who was injured or died from taking the wrong medication.
- The Leapfrog Group, the employer-based patient safety advocacy group, says nearly 98 percent of the hospitals that participated in its 2016 patient safety survey have bar-code medication administration systems to make sure the right patients are getting the right medications in the right doses while in the hospital. But only 30 percent of the hospitals met all four of the group’s criteria for using the systems effectively (bit.ly/2rv30Ke).
- A study in the Journal of the American Medical Association said nearly one-third of the 222 “novel pharmaceuticals and biologics” approved by the Food and Drug Administration from 2001 through 2010 suffered “post-market safety events.” In other words, after the drugs were blessed for use, something bad happened. Three were withdrawn from the market, 61 needed warnings on the box and 59 required safety communications to prescribers (bit.ly/2pww6UL).
- A report from the Pennsylvania Patient Safety Authority says health care facilities in the state cited health information technology as a contributing factor in 889 medication errors from Jan. 1 to June 30, 2016. Technologies like computerized physician order entry and pharmacy automation systems were often to blame for dosage mistakes (bit.ly/2rpnfHa).
- CRICO Strategies, part of the risk management foundation of the Harvard Medical Institutions, analyzed 3,067 malpractice claims and found that 32 percent of the medication-related cases involved a patient death, compared with 18 percent of other types of cases. The three most common drugs in the medication-related malpractice lawsuits were analgesics, anticoagulants and antibiotics (prn.to/2ruo9o1).
- The World Health Organization says medication errors kill at least one person every day in the U.S. and injure 1.3 million people here each year. The WHO estimated the global cost of medication errors at $42 billion annually. In March, it launched its Global Patient Safety Challenge on Medication Safety initiative, with the goal of reducing medication mistakes by 50 percent in five years (bit.ly/2njpPvj).
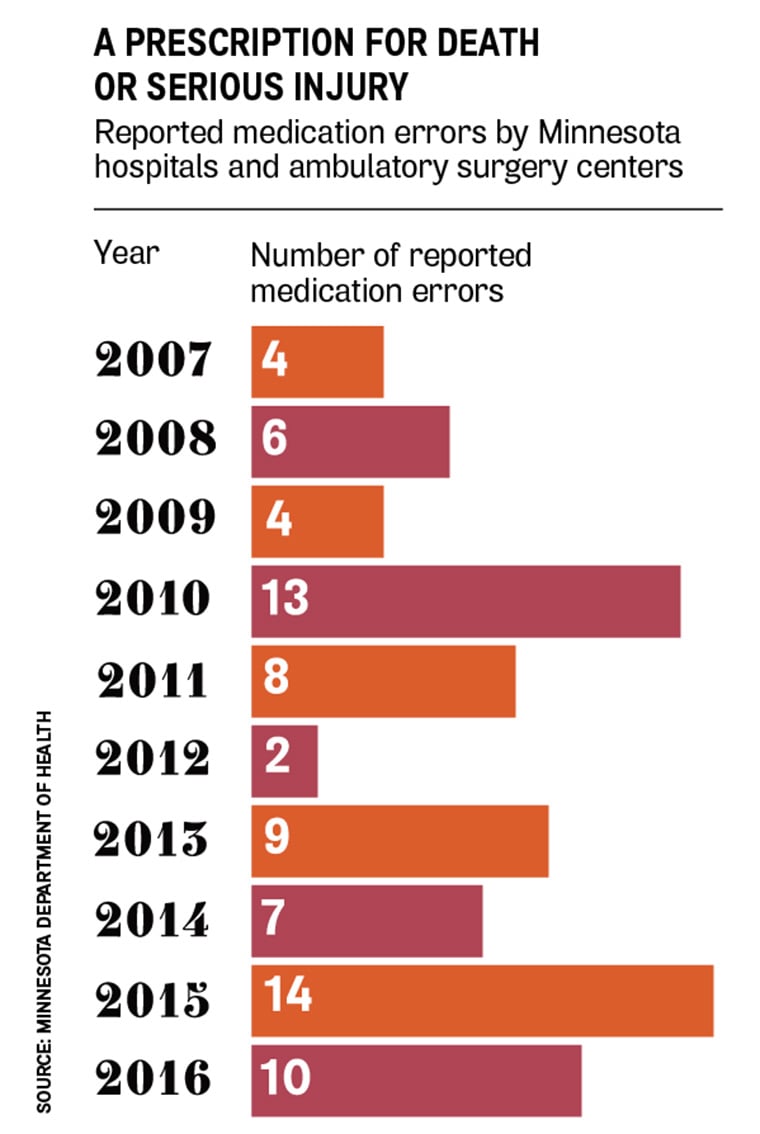
Medication errors accounted for a fraction of the adverse health events reported by Minnesota hospitals and ambulatory surgery centers from Oct. 7, 2015, to Oct. 6, 2016, according to a Minnesota Department of Health report on adverse health events in the state (bit.ly/2mbkkiJ). Only 10 of the 336 adverse health events were medication errors, with one resulting in a patient death. That’s an improvement over the previous reporting year, when the state recorded 14 medication errors, with four resulting in a patient’s death (see chart). Employers should incent their employees through benefits in their health plans to use retail pharmacies, physician practices and hospitals that make medication safety a priority and have a demonstrated and transparent record for medication safety. That’s my prescription, and I hope you get my order right.
David Burda (twitter.com/@davidrburda, dburda@msp-c.com) is editorial director, health care strategies, for MSP-C, where he serves as the chief health care content strategist and health care subject matter expert.
Update
Let’s pretend that a copy of my May column “Mental Health Mindfulness” (bit.ly/2qkPIjm) was magically available to 314 employers last October, and they read it right before they took a survey from Willis Towers Watson. Then, I could take credit for how the employers responded to the survey, which asked them about behavioral health issues in the workplace and how they intend to address the issues. Some 88 percent of the employers said managing the behavioral health of employees is a top priority over the next three years (bit.ly/2qvQ1nC). Specifically:
- 63 percent said they intend to locate more timely and effective treatment of behavioral health issues for their employees
- 61 percent said they intend to integrate behavioral health case management with medical and disability case management for a more holistic view of employee health
- 56 percent said they intend to provide better support for complex behavioral health conditions
- 52 percent said they intend to expand access to behavioral health services
“Employers are concerned about behavioral health issues because of the impact on costs, employee health and productivity, and workplace safety,” Willis Towers Watson said in a release.









