A Hard Look at Minnesota Hospital Finances
The 19-bed rural hospital in Starbuck, Minnesota, where Dr. Rahul Koranne got his start as a physician is no more. Back in 2005, financial pressures forced the small facility to close, leaving the town of about 1,300 without an emergency department. More importantly, Koranne says, the closure left the town without a place for lifelong care.
“That’s what small-town health campuses do,” says Koranne, who worked at the Starbuck hospital from 2000 until 2005 and now serves as president and CEO of the Minnesota Hospital Association. “They take care of the community from birth to death. It’s full service, not just sick care.”
The demise of Starbuck’s lone hospital is not an exception. Koranne believes that scores of other Minnesota cities are likely to endure similar fates in the near future, as their hospitals manage declining revenue and staffing shortages. In his view, it’s a statewide issue that will require buy-in from both the private sector and government. It’s also a trend that predates Covid-19.
“The financials are looking really worrisome,” Koranne says. “Had it not been for the federal government stepping in and supplying grant support, I think [hospitals] would have been in a lot of trouble. … Expenses are going up, and we’re extremely worried about this year and next year.”
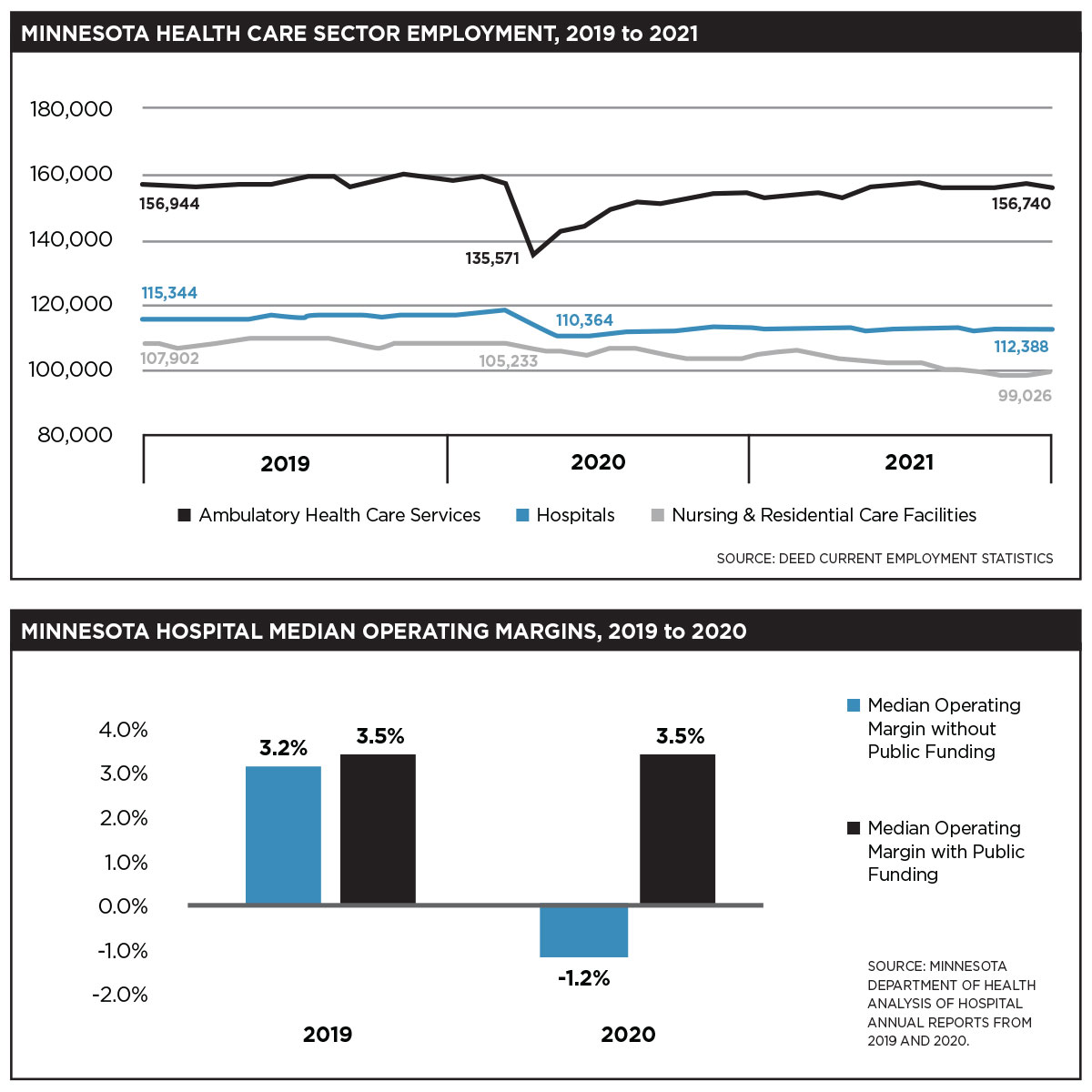
State data corroborates Koranne’s account. According to a March report from the Minnesota Department of Health, public funding for hospitals in the state grew by a whopping 500% in 2020. In Minnesota, hospitals received a total of $879.25 million in 2020, up by $735 million from the prior year. But without that funding, more than half of Minnesota’s 128 hospitals would have operated at a loss, according to the report.
“In 2020, if those funds were removed from the calculation, the median operating margin would drop from 3.5% to -1.2% and over half of Minnesota’s hospitals would be facing negative operating margins,” the report states.
Life after Covid
Covid has burned a serious hole in hospitals’ normal revenue streams. With elective surgeries on pause, hospitals saw a big decline in revenue. Minneapolis-based Fairview Health Services, for instance, lost $57.7 million in 3Q21.
And even if Covid is removed from the picture, the financial situation facing hospitals is still dire, Koranne says. At this point, hospital CEOs he talks with are concerned about a mounting backlog of deferred care for patients. “As patients waited for surgeries, some of their medical conditions have gotten worse,” Koranne says. For hospitals, that’s another big financial risk as patients return for acute care: “That means more complex patient needs, longer hospital stays, and teams of skilled health professionals.”
Of course, financial concerns existed long before Covid struck. Before the pandemic, the median operating margin for Minnesota hospitals was what Koranne calls a “razor-thin” 1.4%.
“We may not be able to serve our patients. It’s that bad. The workforce crisis is that real
for us right now.”—Dr. Rahul Koranne
“That’s not enough money to invest back in the community or in innovations,” he says. “That certainly is not enough money to grow and develop our workforce. And that was before the pandemic.”
The vast majority of Minnesota’s hospitals are nonprofit. MHA has said that a hospital with a 5% operating margin is doing well.
In the first three months of the pandemic, Minnesota hospitals reported a $2.9 billion loss, largely due to the loss of lucrative elective procedures and surgeries. Nonetheless, Koranne is proud of how the state’s health care systems responded. “We did a good job. It wasn’t perfect, but we are absolutely learning from it,” he says.
Misinformation, a hallmark of the pandemic, has been another continued headache for health providers. Fears about vaccines, for instance, have led many individuals to forgo them. Koranne says health care providers have tried to remain steadfast amid a sea of misinformation. “What we have tried to do consistently as the stewards of health is lean on the science,” he says. It’s less about controlling Minnesotans’ individual media habits and more about meeting them where they’re at, in clinics or in hospitals. “We communicate one-on-one every second of every day,” he says. “We are educating and communicating, and that’s a great responsibility.”
A business lens
If there’s anyone suited to take a hard look at the business of health care, it is Koranne. Born in India, he earned his medical degree at the University of Delhi. After a stint in Brooklyn, New York, for a residency in internal medicine, Koranne headed to Minnesota for a fellowship in geriatrics in 1999, which led him to his first role as a physician, in Starbuck.
Read more from this issue
But it was his residency at SUNY Brooklyn that really opened his eyes. At the same time, he did additional work at an area VA hospital. Both experiences shaped his thinking and gave him a window into the business side of health, motivating him to get an MBA in Minnesota.
“I felt that I needed to learn more about the financing of health care, not just the delivery,” Koranne says. “Those two go hand-in-hand. If the financing is off, or if it doesn’t serve and support the delivery, then you can’t really do the best job for the population that you’re serving. It’s that marriage.”
For Koranne, the closure of the Starbuck hospital laid bare the fragility of health care finances. That’s part of the reason he returned to school to earn his MBA from the University of Minnesota’s Carlson School of Management in 2008. He’s also taught courses on medical finances at Carlson for the last 10 years. “In medicine, we are not trained in finances as much as we should [be],” Koranne says.
Public funds needed
In Koranne’s view, government aid will be critical in helping hospitals dig out of their financial woes. “No question about it: We are going to need external help from the government,” he says.
Medicare is already the largest payer in the United States, serving more than 63 million individuals. It’s a trend that doesn’t appear to be slowing anytime soon, Koranne says.
The MHA is also “strongly advocating” for another round of Covid-19 health care grants. In spring of 2020, Minnesota lawmakers authorized $200 million to help providers with pandemic-related expenses. Koranne notes that there wasn’t any additional state funding for Covid-related expenses after that, “despite high numbers of Covid-19 patients” in 2021.
“We are pleading for help,” Koranne says. “If that fragility of the financials is not attended to, I’m extremely worried about what that would mean to access to quality care in all of our communities.”
He concedes that Minnesota’s hospitals have received a number of federal grants, but he maintains that they’ll still need “stabilizing” from the federal government in the years ahead.
Financing is, of course, just one piece of the puzzle. The other looming concern is a growing workforce shortage. Despite the countless headlines about hospital bed shortages across the state throughout the pandemic, Koranne argues that workforce is a bigger concern than physical capacity. It’s the absence of nurses, support staff, and doctors that may lead to dire consequences down the road.
Now hiring
Hospitals might be forced to reduce services if staffing doesn’t pick up, Koranne says. “We may not be able to serve our patients. It’s that bad. The workforce crisis is that real for us right now.”
According to data from the Minnesota Department of Employment and Economic Development (DEED), there were about 40,000 job vacancies in the health care and social assistance sector in 2Q21—one of every five job vacancies in Minnesota.
“This is the largest number of vacancies ever reported, surpassing the peak set in the fourth quarter of 2020,” said a 2021 DEED report.
According to DEED, about 112,000 people were working in hospitals at the end of 2021, down from 115,344 in January 2019. And that’s just in hospitals: 471,300 people were working in the entire health care and social assistance sector in the state at the start of 2022.
What types of jobs are going unfilled? They run the gamut, touching everything from personal care aides to certified nursing assistants and registered nurses. There were more than 9,200 openings for home health and personal care aides alone in 2Q21.
“With all these positions open, we have got to make it easy for Minnesotans graduating from a medical school, physical therapy school, or nursing school to join the health care system here,” Koranne says. “We’ve got to make it seamless. We’ve got to make it easy. We shouldn’t even let a single Minnesota health care graduate think about leaving Minnesota.”
That’s part of the reason the hospital association is partnering with nonprofit health insurer UCare to develop a “first-of-its-kind road map for health care workforce development.” That plan is slated to be complete in 2022, and Koranne is already thinking about possible solutions. Better loan-forgiveness programs, for example, may help entice some workers to stay in Minnesota. There may even be opportunities to attract potential workers long before they start their formal medical education.
Koranne maintains that the pandemic accelerated the health care industry’s existing workforce shortage. “Many individuals decided to retire early, experienced unforeseen burnout, and others simply wanted to pursue other passions,” he says. “Health care was not immune to what every other industry is currently feeling.
“How do we inculcate in the K-12 schooling system an understanding of what this calling is all about? We’re going all the way back to kindergarten and starting to think about how we can work with school systems,” Koranne says. “We want to grow and strengthen the pipeline.”
This article appeared in the April/May 2022 issue with the headline “The Hospital Sickness.”









