Mental Health Mindfulness
Let’s pretend there was overwhelming reader response to my series of columns urging employers to take an active role in helping workers manage their mental health. Employers big and small, near and far, are clamoring for more information on how to deal with the challenges of mental illness at work.
“Dave, please, please share any information you have on workplace mental illness rates and employee mental health benefits,” they write, always adding a few lines about how much they love my column.
So I will oblige. Thanks to a survey of 247 U.S. employers by the International Foundation of Employee Benefit Plans (IFEBP), I have some of the answers you’ve been seeking (bit.ly/2n8kh6n). But first, a little stage-setting, in case there are a few of you who need to get caught up:
In November, we talked about how reducing workplace stress can improve productivity (bit.ly/2elJLM0).
In September, we talked about helping workers get rid of those unused opioid prescriptions (bit.ly/2cO999k).
And in June, we talked about why it was important to promote routine screening of employees for depression (bit.ly/2kJQEuE).
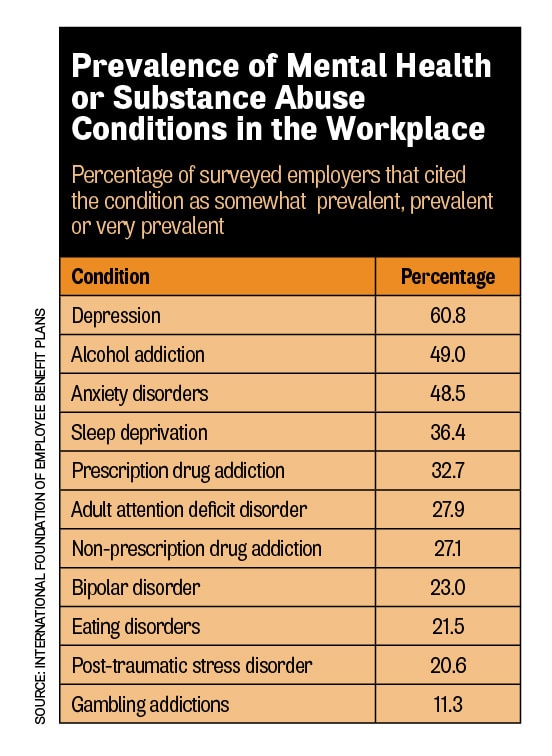
Here’s why it’s important for employers to take those issues seriously. More than one-third of the employers surveyed by the IFEBP said 11 to 30 percent of their workforce suffered from mental health or substance abuse issues. The five mental health or substance abuse conditions most often cited by the respondents as prevalent in their workplaces were depression, alcohol addiction, anxiety disorders, sleep deprivation, and prescription drug addiction (see chart). A whopping 94.3 percent of the employers said their employees were somewhat, very or extremely stressed.
The problems are costing businesses in lost productivity and higher health care costs. The top five consequences cited by the respondents were absenteeism/tardiness, overall job performance, poor physical health, inability to focus on work/productivity, and relationships with co-workers. The employers said 13.6 percent of their health care costs were attributable to mental health or substance abuse issues.
Although most employers said they offered medical benefits that cover mental health or substance abuse treatments, most employers don’t go beyond employee assistance programs (EAPs) to help workers avoid the problems in the first place.
For example, 89.9 percent of the employers said they cover outpatient mental health treatment, 84.1 percent said they cover inpatient mental health care and 80.2 percent said they cover prescription drug therapy. About 89 percent said they cover outpatient substance abuse care, 84.6 percent said they cover inpatient substance abuse care and 67 percent said they cover prescription drug therapies for substance abuse.
But after EAPs (88.1 percent), less than half said they offer mental health/substance abuse wellness programs (40.1 percent), mental health/substance abuse risk assessments (29.5 percent), stress management programs (26.9 percent), mindfulness/meditation resources (19.4 percent) or gratitude/appreciation initiatives (4 percent).
I don’t know what formal gratitude or appreciation initiatives are, but even if they involved a chocolate cake with buttercream frosting, I’m not sure employees would take advantage of them. The No. 1 barrier to workplace mental health or substance abuse initiatives, according to the survey, is the fear that admitting a problem will put the worker’s job security at risk.
Culture starts at the top. But so does the buck for the balance sheet. Employers that want to reduce their health care costs and increase employee productivity should make improving mental health and reducing substance abuse cornerstones of their workplace wellness programs.
Short Take
The Minnesota Department of Health’s most recent report on adverse health events in the state is your classic good news/bad news story for patients and those who pay their health care bills (bit.ly/2mbkkiJ). The good news: Only four patients died from medical mistakes at hospitals and ambulatory surgery centers (ASCs) from Oct. 7, 2015, through Oct. 6, 2016. That’s down 75 percent from 16 patient deaths the previous reporting year. The bad news: The total number of mistakes reported to the state by hospitals and ASCs rose 6.3 percent to 336 from 316. Of the 29 different types of adverse health events reported to the state, most of the ones that occurred last year—nearly 60 percent—were pressure ulcers and patient falls. Of most interest to me as a patient—and what should be of most interest to employers—were the really scary mistakes. That and the fact that hospitals and ASCs really didn’t move the needle on these really scary mistakes in the right direction between the previous two reporting years:
- The number of wrong-site surgeries rose by one to 30 from 29.
- The number of irretrievable losses of irreplaceable biological specimens rose to 31 from 27.
- The number of times foreign bodies were left inside surgical patients rose to 26 from 22.
- The number of wrong surgeries or invasive procedures dipped by one to 19 from 20.
- The number of medication errors declined by four to 10 from 14.
Let’s take our hats off to the state for requiring hospitals and ASCs to report this information. Let’s take our hats off to hospitals and ASCs for being transparent about their mistakes and reporting them to the state and to the public. But with 41 percent of the mistakes caused by rules, policies and procedures (or people not following them), there’s no excuse for the really scary mistakes to be happening. As we’ve mentioned in previous columns, employers should be steering their workers to the safest hospitals and ASCs, and the ones that have corrected these correctable errors (bit.ly/1OAg872).
David Burda (twitter.com/@davidrburda, dburda@msp-c.com) is editorial director, health care strategies, for MSP-C, where he serves as the chief health care content strategist and health care subject matter expert.









