Long-Term Impact: Fairview Health Services
Fairview Health Services’ approach to care should be far more commonplace, says Cristina Flood Urdangarin.
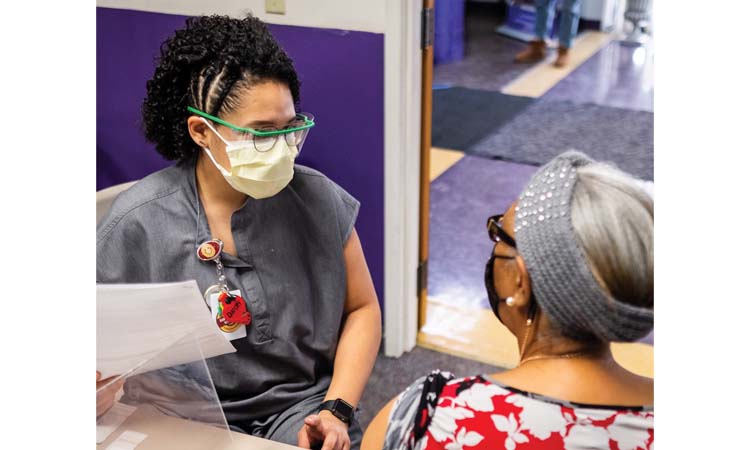
A physician, Flood Urdangarin has worked at the St. Paul-based St. Mary’s Health Clinics since 2002. The community health outreach manager, she partners with Fairview Health Services on free vaccinations. This is through Fairview’s Minnesota Immunization Networking Initiative (MINI), which sets up in community settings—schools, churches, mosques, community centers. Besides vaccinations, the program, launched in 2006, provides blood pressure checks and other health services and education to low-income and uninsured people.

The partnership with St. Mary’s Health Clinics is one of the ways that Fairview connects with the Latino community. “We went to the Latino churches after Mass, because it was important to have the family together,” Flood Urdangarin says. St. Mary’s has “connections with the sites, with the churches, with the schools,” she adds. “They trust us because we have a relationship with them.”
What’s the impact? Last year, Fairview administered, among other vaccines, more than 6,190 flu shots at 443 community-based events.
“The MINI project is such a successful model that it should be replicated,” Flood Urdangarin says.
And it’s only one example of Fairview’s reach. More than a decade ago, Fairview launched Community Advancement to formally recognize three ideas: “Food Is Medicine,” “Housing Is Health,” and “Connection Is Cure.” By emphasizing these three principles in its programs, Fairview has had a measurable impact in improving the health of Minnesotans. In 2024, Fairview’s total investment in community was $1.4 billion, including community benefit and other contributions such as care provided without compensation and discounts to uninsured patients.
“If you would have told me 15 years ago that we [at Fairview] would be working on ‘Food Is Medicine’ and farm bills and things like that, I probably would have scratched my head,” says John Swanholm, Fairview’s vice president of community advancement. In his 22 years with Fairview, the provider has “evolved to become much more focused on ‘upstream’ work—like let’s keep people out of the hospital.”

Today, that approach isn’t so strange. A 2016 study published in the American Journal of Preventive Medicine suggests social factors influence health far more than clinical care does. Socioeconomic determinants, health behaviors, and physical environment account for nearly 85% of health outcomes, the study says. Clinical care makes up the rest.
Two years ago, Fairview rolled out food insecurity screenings—as part of its social determinants of health screening approach—across its primary care practices. Patients are asked, for example, whether they feel confident they have enough food for the month. From there, “resource navigators” can help overcome barriers to accessing nutritious food, such as transportation.
Last year, Fairview also launched Fair Table. To expand food access for people, about 100,000 pounds of food, on average, were packaged weekly through the Fairview Community Health and Wellness Hub.
Terese Hill oversees Fair Table. In early September, she was anticipating greater food needs because of SNAP (food assistance) reductions contained in a recent bill Congress passed. “As the initiative has grown, we’ve also gotten more connected with policymakers and other levers,” she says.
Those community roots help explain Fairview’s status as an anchor institution. “We all have our roles, and they respect us,” Flood Urdangarin says of Fairview staff. “They build on the skills and gifts everybody has.”